© 2025 NH SRCC Children's Hospital. All Rights Reserved.
Powered By VCOGS DIGITAL MEDIA
Autoinflammatory diseases are rare, chronic conditions caused by a malfunction in the innate immune system—your body’s initial defense mechanism. Unlike autoimmune disorders, where the body creates antibodies that attack its own healthy tissues, autoinflammatory conditions are caused by internal signaling errors that trigger severe, unprovoked episodes of widespread inflammation.
While many of these conditions are diagnosed in childhood, some can persist into adulthood, and others—like Adult-Onset Still's Disease—can appear for the first time later in life. Because the symptoms often mimic severe infections or malignancies, obtaining an accurate diagnosis can be a frustrating and lengthy process.
Adults suffering from undiagnosed autoinflammatory conditions often endure years of episodic illnesses. Left untreated, systemic chronic inflammation can lead to severe, irreversible complications:
Chronic inflammation can slow bone and overall physical development.
Prolonged untreated disease may affect organs like the liver, kidneys, or heart.
Continuous inflammation often leaves children feeling weak and drained.
Frequent illness and discomfort disrupt education and friendships.
Persistent pain and limitations can impact overall well-being and happiness.
Adult-Onset Still’s Disease (AOSD):
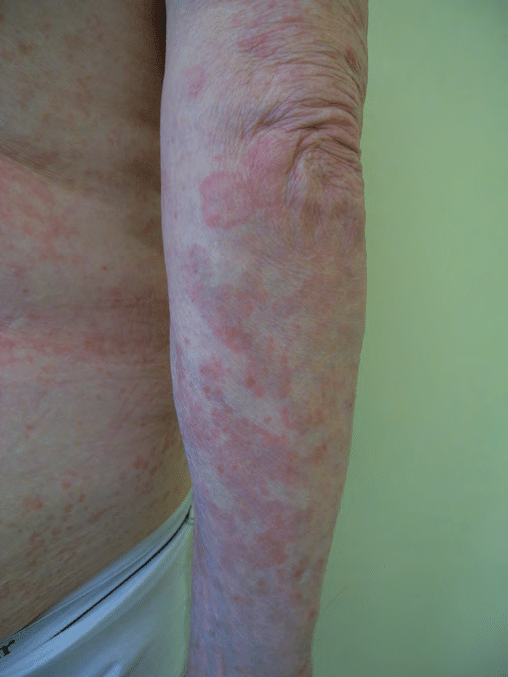
A rare systemic inflammatory disease characterized by high spiking fevers, transient salmon-colored rashes, and severe joint pain.
FMF (Familial Mediterranean Fever)
A genetic disorder that can persist into or occasionally present in adulthood, leading to sudden, severe fever episodes accompanied by painful inflammation in the abdomen, chest, or joints.
TRAPS (TNF Receptor-Associated Periodic Syndrome)
A group of genetic disorders marked by recurrent fevers, rashes, and risk of hearing or vision problems.
TRAPS (TNF Receptor-Associated Periodic Syndrome)
A condition causing prolonged fever episodes lasting weeks, accompanied by severe muscle pain, abdominal pain, and migrating skin rashes.
CAPS (Cryopyrin-Associated Periodic Syndromes)
A spectrum of rare diseases that can cause daily fevers, hives-like rashes, joint pain, and long-term risks of hearing loss or kidney issues.
Behçet’s Disease
Often sharing autoinflammatory characteristics, this condition causes recurrent painful oral and genital ulcers, eye inflammation, and skin lesions.
With years of clinical excellence, Dr. Pallavi Pimpale is a trusted expert in treating complex rheumatological and autoinflammatory disorders in both pediatric and adult patients at the PREP Clinic.
Fevers lasting 3–7 days, returning every few weeks or months.
Do not improve with antibiotics.
Common in PFAPA, CAPS, TRAPS, and similar conditions.
Painful, recurring sores inside the mouth. Often accompanied by sore throat and fever.
Most noticeable in the neck region.
Tender during flares but usually without infection.
Sudden red, non-itchy rashes.
Typically fade after the fever or flare resolves.
Recurrent pain without digestive or respiratory cause.
Common in FMF and other periodic fever syndromes.
Pain or stiffness during or after fever episodes.
Can occur even without visible swelling.
Do not ignore recurrent, unexplained symptoms. If you experience any of the following warning signs, schedule a consultation with a rheumatologist to secure an accurate diagnosis and prevent long-term complications:
You should schedule an appointment with a rheumatologist if you notice any of the following:
Fevers of Unknown Origin (FUO): Recurrent high fevers that last for days or weeks and do not respond to standard antibiotics.
Unexplained Joint & Muscle Issues: Sudden, severe joint pain, swelling, and stiffness, or profound muscle weakness during fever episodes.
Skin Rashes: Rashes that appear and disappear alongside your fevers, or persistent hives that do not itch.
Chest & Abdominal Pain: Recurrent, severe stomach or chest pain without a clear digestive or cardiac cause (serositis).
Mouth Ulcers & Gland Swelling: Frequent, painful mouth ulcers or unexplained swelling of the lymph nodes in your neck.
Early evaluation by a rheumatologist helps in accurate diagnosis, timely treatment, and prevention of long-term joint or organ damage.
Adult autoinflammatory diseases often present as diagnostic dilemmas. Early recognition and timely referral to a rheumatology specialist are critical to preventing irreversible organ damage, such as secondary amyloidosis or macrophage activation syndrome (MAS).
Please consider a referral to PREP Clinic if your adult patient presents with:
Fevers of Unknown Origin (FUO): Unresponsive to empirical antibiotics.
Persistently Elevated Acute Phase Reactants: Consistently elevated CRP, ESR, or Ferritin without clear evidence of infection or malignancy.
Recurrent Serositis: Episodes of sterile peritonitis, pleuritis, or pericarditis.
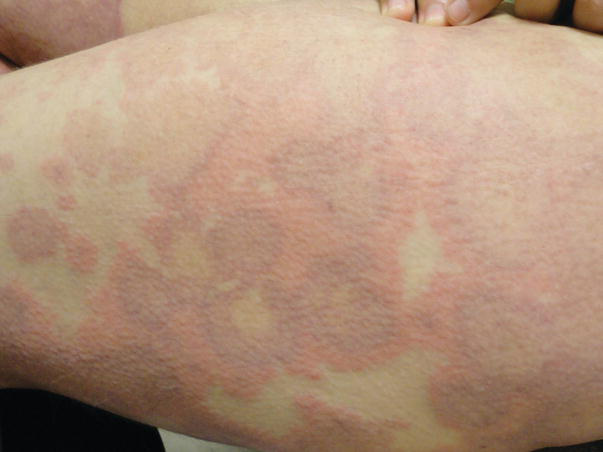
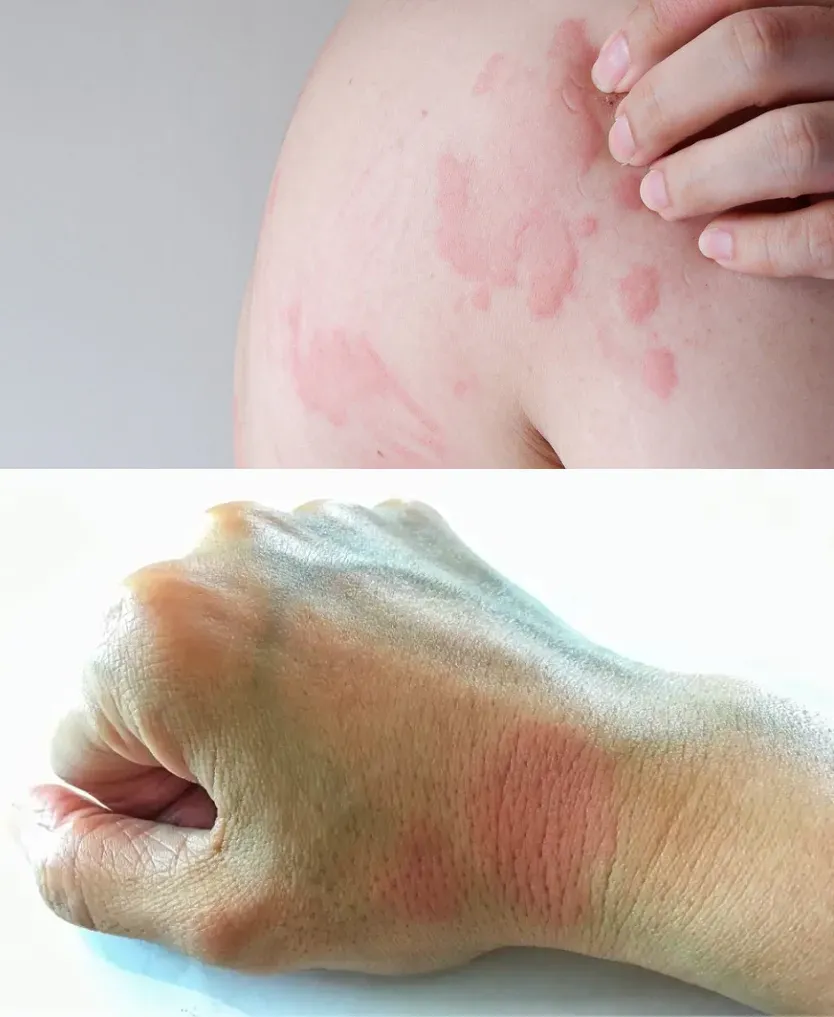
Evanescent Rashes: Rashes coinciding with fever spikes.
Chronic Fatigue with Severe Arthralgia/Arthritis: Unexplained fatigue combined with significant joint pain or inflammation.
Early referral ensures a comprehensive evaluation, targeted genetic or clinical diagnosis, and the initiation of biologic or targeted therapies for your patients.

Dr. Pallavi Pimpale is a skilled Pediatric Rheumatologist specializing in autoinflammatory diseases, offering expert care with global experience and advanced research in genetic and molecular diagnostics.
Powered By VCOGS DIGITAL MEDIA